The following is a naturopathic case report summary of a patient with rashes, and no overtly apparent cause. She received nutrients, medications, and dietary counseling from a naturopathic doctor overseeing her care. There are many layers of a naturopathic approach to and this is just one of the many ways these types of symptoms can be diagnosed and treated. This case report is for informational purposes only and should not be used to diagnose or self-treat for this or any other condition.
Here’s What We Know
- Unexplained rashes may be a symptom of a larger health issue.
- Gut microbiome imbalance may cause symptoms that show up outside of the digestive system.
Hypothesis for Treatment: Under a doctor’s recommendation, restoring the microbiome imbalance (when bad gut bacteria outnumber good gut bacteria) with nutrients, medications, and dietary changes, may safely resolve unexplained skin rashes.*
An Itchy, Burning Rash That Spread Across Her Body
When 32-year-old LS** first came to see Dr. Alisha Ghajar, ND, she was frustrated.
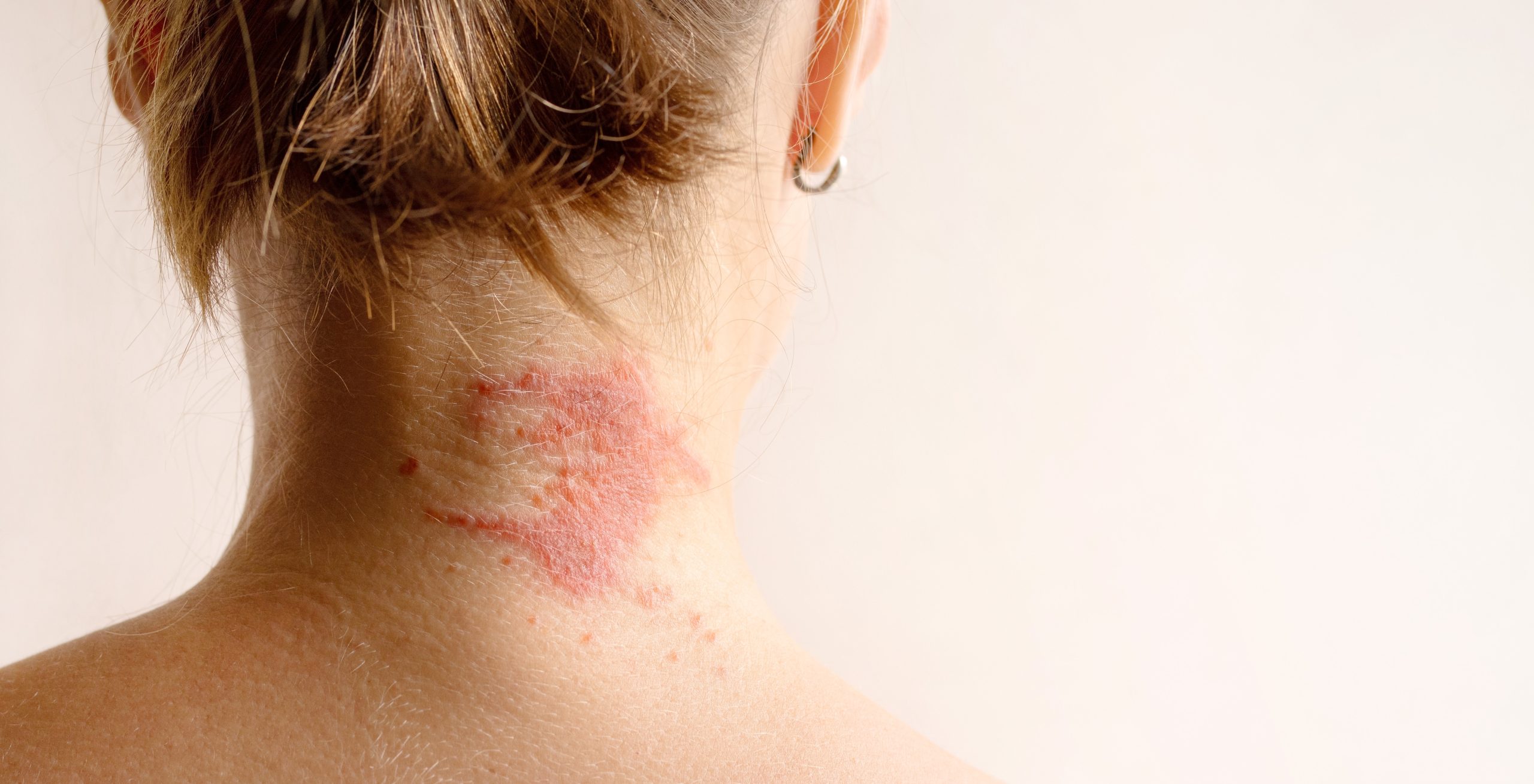
One month earlier, LS awoke with a red, itching, burning rash on her neck and hands. She had eaten Thai food the night before, but that was nothing unusual. She often enjoyed this spicy cuisine. Over the past month, the rash had slowly spread to the rest of her body.
When an internist prescribed steroid medication in both pill and cream form. LS declined the pill. And although she used the cream, she only gained minimal relief.
LS noticed her rash worsened after eating spicy foods, during times of stress, and when her body became overheated. She found temporary relief by applying moisturizers, ice packs and taking cold showers.
Delving into her past, Dr. Ghajar could not see a history of rashes or extreme allergic reactions (anaphylaxis). One year earlier, LS woke up vomiting almost every morning for a month. An internist ruled out pregnancy, appendicitis, and gallstones. Thorough blood testing was done, which came back normal. Unfortunately, by the time she got an appointment with a gastroenterologist, her symptoms had disappeared, and she did not pursue further testing.
During this first appointment, LS reported several symptoms in addition to the rash. She was frequently tired, and her migraines were getting worse. She couldn’t think clearly, felt light-headed, and had chemical sensitivities (chemicals such as paint and perfume may cause headaches, brain fog, and other symptoms). She had a history of summer allergies. Particularly troubling, she would wake up vomiting once or twice a week, every three to four weeks. At times, she felt a sharp stomach pain after eating, which would last for a few minutes.
Despite the stomach pains, Dr. Ghajar noted LS was not experiencing constipation, diarrhea, or heartburn when assessing digestive symptoms.
When assessing potential food allergies, Dr. Ghajar noted her diet was varied, with no food restrictions. She did not experience severe allergic reactions such as shortness of breath or swelling of her eyes, throat, or tongue.
When looking at her chemical sensitivities, Dr. Ghajar noted LS used only unscented cleaning products and laundry detergent designed for sensitive skin. LS told her doctor that she had not started using any new personal care products.
LS worked from home for a software company and had not recently traveled. She lived with her partner, who reported no illness or rashes.
Her physician’s complete physical exam revealed a red rash across her entire body, including the palms of her hands and soles of her feet. Only her face was spared. Except for frequent throat clearing and a mild cough when laughing, all other exam findings were normal.
What Happens in the Gut, May Not Stay in the Gut
Dr. Ghajar gained a great deal of information at this first visit. But there were more questions than answers. Dr. Ghajar took all her symptoms and history into account explored a few potential causes.
Could the rash result from an allergy to foods like gluten, or another substance? Due to her ongoing nausea and vomiting, Dr. Ghajar also suspected an imbalance in her gut microbiome. It is common that when bad gut bacteria outnumber good gut bacteria, a gut-related infection could be a factor.
To narrow down the options, Dr. Ghajar ordered a lab test to assess whether she had celiac disease (when eating gluten over stimulates the immune system and causes small intestine damage). She also ordered a DNA stool test to see what was going on in her gut.
LS did not have insurance at the time, so the cost was a concern. Until the test results came back to shed more light on the potential causes of the rash, Dr. Ghajar advised LS to take over-the-counter allergy medications loratadine (Claritin) or diphenhydramine (Benadryl) daily, which would test whether seasonal allergies were contributing to the rash.
When LS returned for her second visit two weeks later, she reported mixed results. The good news? She hadn’t experienced any nausea or vomiting. The bad news? Although taking diphenhydramine every night eased the rash for a short time, it was no longer working.
Dr. Ghajar also had news to share. The lab test results were back, celiac disease was ruled out. LS’ recent experience also ruled out seasonal allergies. The DNA stool test was more telling. It turns out that LS had an H. Pylori (bacterial) infection. No antibiotic-resistant genes were identified, which means that the strain of H. Pylori in her gut would likely respond well to antibiotic treatment.
H. Pylori is best known for raising peptic ulcer risk. It weakens the stomach lining and the first part of the small intestine, allowing acid to enter causing ulcers to develop. But LS had seen other doctors – how did they miss this bacterial infection?
Dr. Ghajar knew that in conventional medicine, doctors are unlikely to test for H. Pylori unless the patient shows signs of peptic ulcers. She also knew several studies had linked skin diseases like rosacea and psoriasis with H. Pylori infections.
With a new focus on H. Pylori, Dr. Ghajar advised LS of two treatment options: an herbal combination or triple therapy (the first-line conventional treatment that is a combination of antibiotics and medications that reduce stomach acid).
LS was in significant discomfort from the rash and preferred pharmaceutical treatment. By this time, she had secured insurance which included drug coverage, but it did not cover herbal therapies. LS opted for triple therapy and was prescribed a combination of three medications— clarithromycin, metronidazole and omeprazole, for two weeks.
Dr. Ghajar also knew that H. Pylori could form biofilms – a sticky layer that protects bacteria from the body’s efforts to get rid of them. Research shows that biofilms can make bacterial infections harder to treat by making them resistant to antibiotics and generally allowing bacterial growth to get out of control. Although the DNA stool test showed that LS was not harboring antibiotic-resistant H. Pylori, she was keen to address the potential impact of biofilms. Dr. Ghajar prescribed a supplement containing a mix of enzymes designed to eradicate existing biofilms and prevent new ones from forming.
Dr. Ghajar also advised LS to support her liver’s detoxification abilities by cutting out processed foods and alcohol, and eating more cruciferous vegetables (like broccoli and cabbage), whole grains and grass-fed, free-range protein.
But Dr. Ghajar didn’t rule out that her rash was solely related to H. Pylori, at least not just yet. With the celiac disease testing coming back negative, she ordered more testing to explore the potential role of other food allergies.
At her third visit two weeks later, LS had excellent news. Her rash had started to clear up after just one week of treatment, and only remained on the palms of her hands and her legs. It wasn’t just the rash that had improved; her cough was gone, and she no longer needed to clear her throat frequently.
The food sensitivity testing came back with good news—no food allergies were identified. Best of all, Dr. Ghajar performed a breath test which showed that LS no longer had an H. Pylori infection.
At the final visit two weeks later, LS was still going strong. The nausea and vomiting had not returned. Most importantly, the rash was completely gone from all areas of her body.
How a Naturopathic Doctor May Address Unexplained Rashes
In cases of unexplained rashes where gut microbiome imbalance is a factor, a targeted combination of nutrients, medications and dietary changes may safely clear up rashes.
After six weeks of naturopathic treatment, LS’ full-body rash (and the itching and burning sensations) are entirely gone. The troubling nausea and vomiting has not returned, and her cough was resolved.
Editor’s Note
This case report is not meant to diagnose or treat rashes or any other disease. It is provided for educational purposes only. This case report is a short summary of one treatment for one patient’s experience and does not reflect a comprehensive naturopathic approach to rashes. Naturopathic medicine is designed to treat each person individually with whole person care If you are experiencing health issues that need treatment, please consult with a naturopathic doctor right away.
What does LS’ case tell us about Naturopathic Medicine and unexplained rashes? Here are some key takeaways:
Naturopathic doctors work with patients to find affordable treatment recommendations. LS’ lack of health insurance in the United States (at the first visit) limited which lab tests could be ordered. Fortunately, LS negotiated lower cost cash-pay labs for some of the tests. When LS did secure insurance, it did not cover herbal treatments. The instead prescribed triple therapy, was both effective and covered by her insurance.
Naturopathic doctors listen carefully to all symptoms and consider them into account when exploring diagnosis options. LS had very few signs, symptoms, or risk factors for H. pylori infection. The American College of Gastroenterology released a 2017 guideline for the “Treatment of Helicobacter pylori infection”. Unfortunately, LS would not have qualified for testing under these guidelines. It is only due to the naturopathic principle of Treat the Whole Person that the off-handed mention of intermittent nausea and vomiting was considered a factor for her rash. Indeed, prior medical visits resulted in steroid prescriptions to suppress inflammation without digging deeper.
Naturopathic doctors know how to combine pharmaceutical and natural treatment options for complete patient care. Although triple therapy is the gold standard treatment for H. pylori infections, Dr. Ghajar didn’t stop there. Adding an enzyme supplement to rid biofilms and making dietary recommendations to support detoxification represents a truly personalized, integrative medicine approach.
“There are over 500,000 people estimated to have chronic urticaria (hives) in the United States,” according to research. Are you wondering if a naturopathic therapy may help you or your loved ones with unexplained rashes? A naturopathic doctor can help. Find a Naturopathic Doctor in your area with our Find an ND search portal.
Clinical References from Dr. Ghajar, ND
- Chey, W. D., Leontiadis, G. I., Howden, C. W., & Moss, S. F. (2017). ACG Clinical Guideline: Treatment of Helicobacter pylori Infection. American Journal of Gastroenterology, 112(2), 212–239. https://doi.org/10.1038/ajg.2016.563
- Chey, W. D., Leontiadis, G. I., et al (2017). ACG Clinical Guideline: Treatment of Helicobacter pylori Infection. American Journal of Gastroenterology, 112(2), 212-239. doi:10.1038/ajg.2016.563
- Connor, B. (2017). Helicobacter pylori – Chapter 4 – 2020 Yellow Book | Travelers’ Health | CDC. Cdc.gov; CDC.gov. Retrieved Sept. 11,2020, from https://wwwnc.cdc.gov/travel/yellowbook/2020/travel-related-infectious-diseases/helicobacter-pylori
- Gravina, A. G., Zagari, R. M., De Musis, C., Romano, L., Loguercio, C., & Romano, M.
(2018). Helicobacter pylori and extragastric diseases: A review. World journal of
Gastroenterology, 24(29), 3204–3221. https://doi.org/10.3748/wjg.v24.i29.3204
Clinical References from the Editor
- Baj, J., Forma, A., Flieger, W., Morawska, I., Michalski, A., Buszewicz, G., Sitarz, E., Portincasa, P., Garruti, G., Flieger, M., & Teresiński, G. (2021). Helicobacter pylori Infection and Extragastric Diseases—A Focus on the Central Nervous System. Cells, 10(9), 2191. https://doi.org/10.3390/cells10092191
- Cui, Y.-L., Zhou, B.-Y., & Gao, G.-C. (2021). A systematic review and meta-analysis of the correlation between Helicobacter pylori infection and chronic urticaria. Annals of Palliative Medicine, 10(10), 10584–10590. https://doi.org/10.21037/apm-21-2324
- Essrani, R., Sullivan, M., & Shah, H. (2019). Chronic Urticaria Associated with Helicobacter pylori. Cureus. https://doi.org/10.7759/cureus.4528
- Fauzia, K. A., Miftahussurur, M., Syam, A. F., Waskito, L. A., Doohan, D., Rezkitha, Y. A. A., Matsumoto, T., Tuan, V. P., Akada, J., Yonezawa, H., Kamiya, S., & Yamaoka, Y. (2020). Biofilm Formation and Antibiotic Resistance Phenotype of Helicobacter pylori Clinical Isolates. Toxins, 12(8), 473. https://doi.org/10.3390/toxins12080473
- Gravina, A. G., Priadko, K., Ciamarra, P., Granata, L., Facchiano, A., Miranda, A., Dallio, M., Federico, A., & Romano, M. (2020a). Extra-Gastric Manifestations of Helicobacter pylori Infection. Journal of Clinical Medicine, 9(12). https://doi.org/10.3390/jcm9123887
- Gravina, A. G., Priadko, K., Ciamarra, P., Granata, L., Facchiano, A., Miranda, A., Dallio, M., Federico, A., & Romano, M. (2020b). Extra-Gastric Manifestations of Helicobacter pylori Infection. Journal of Clinical Medicine, 9(12). https://doi.org/10.3390/jcm9123887
- Guarneri, C., Ceccarelli, M., Rinaldi, L., Cacopardo, B., Nunnari, G., & Guarneri, F. (2020). Helicobacter pylori and skin disorders: a comprehensive review of the available literature. Eur Rev Med Pharmacol Sci., 24(23), 12267–12287. https://doi.org/10.26355/eurrev_202012_24019
- Hathroubi, S., Servetas, S. L., Windham, I., Merrell, D. S., & Ottemann, K. M. (2018). Helicobacter pyloriBiofilm Formation and Its Potential Role in Pathogenesis. Microbiology and Molecular Biology Reviews, 82(2). https://doi.org/10.1128/mmbr.00001-18
- Krzyżek, P., Grande, R., Migdał, P., Paluch, E., & Gościniak, G. (2020). Biofilm Formation as a Complex Result of Virulence and Adaptive Responses of Helicobacter pylori. Pathogens, 9(12), 1062. https://doi.org/10.3390/pathogens9121062
- Lewinska, A., & Wnuk, M. (2017). Helicobacter pylori-induced premature senescence of extragastric cells may contribute to chronic skin diseases. Biogerontology, 18(2), 293–299. https://doi.org/10.1007/s10522-017-9676-x
- Santos, M. L. C., Brito, B. B. de, Silva, F. A. F. da, Sampaio, M. M., Marques, H. S., Silva, N. O. e, Queiroz, D. M. de M., & Melo, F. F. de. (2020). Helicobacter pylori infection: Beyond gastric manifestations. World Journal of Gastroenterology, 26(28), 4076–4093. https://doi.org/10.3748/wjg.v26.i28.4076
- Zhang, C., & Wei, Y. (2021). Association Between Helicobacter pylori-Negative Peptic Ulcer Disease and Chronic Urticaria: A Retrospective Observational Study. Clinical, Cosmetic and Investigational Dermatology, Volume 14(14), 1637–1643. https://doi.org/10.2147/ccid.s336617